Flexible Addiction Treatment: Outpatient Recovery Programs

Key Takeaways: Your Decision Roadmap
Before diving into the details, here is a quick decision guide to help you navigate your options:
- Assess Your Schedule: Use the comparison table in Section 1 to decide between PHP (daily structure), IOP (3-5 days/week), or OP (weekly check-ins) based on your work and family commitments.
- Verify the Toolkit: Ensure your chosen provider offers evidence-based therapies like CBT and DBT. Metrics show these specific therapies increase treatment retention by over 30%.
- Plan the Logistics: Your immediate next action is to call two providers and ask specifically about "integrated care" for co-occurring conditions and their specific insurance payment plans.
Understanding Outpatient Recovery Foundations
Finding the right outpatient recovery program Portland area offers a flexible path to healing that allows you to maintain your daily responsibilities while receiving professional support. Unlike residential treatment, outpatient care provides structured therapy sessions and medical oversight while you continue living at home, working, and staying connected with your support systems.
The foundation of effective outpatient recovery rests on three core pillars:
- Consistent Therapeutic Engagement: Regular interaction with counselors to build coping mechanisms.
- Medical Monitoring: Oversight for medication and physical health when needed.
- Community Support: Connection with peers who understand the journey.
These programs typically involve multiple weekly sessions that include individual counseling, group therapy, and educational workshops designed to build lasting recovery skills. What makes outpatient treatment particularly effective is its real-world application. You immediately practice coping strategies in your actual environment, learning to navigate triggers and challenges as they arise. This approach builds resilience and confidence in ways that feel authentic and sustainable.
Outpatient programs serve various needs, from those beginning their recovery journey to individuals transitioning from higher levels of care. The intensity can be adjusted based on progress and individual circumstances, ranging from several hours per week to more intensive daily programming. This adaptability ensures that treatment evolves alongside your recovery, providing the right level of support at each stage of the healing process.
What Makes Outpatient Treatment Effective
What you’ll learn: This section reveals the key ingredients that make outpatient treatment effective and how you’ll recognize real progress in your recovery or that of a loved one. You’ll be able to spot the difference between an average and an exceptional program based on results and support.
Outpatient recovery works because it combines flexibility with evidence-based support. Think of it as building a sturdy bridge: each element—medical care, therapy, peer groups, and family support—adds strength.
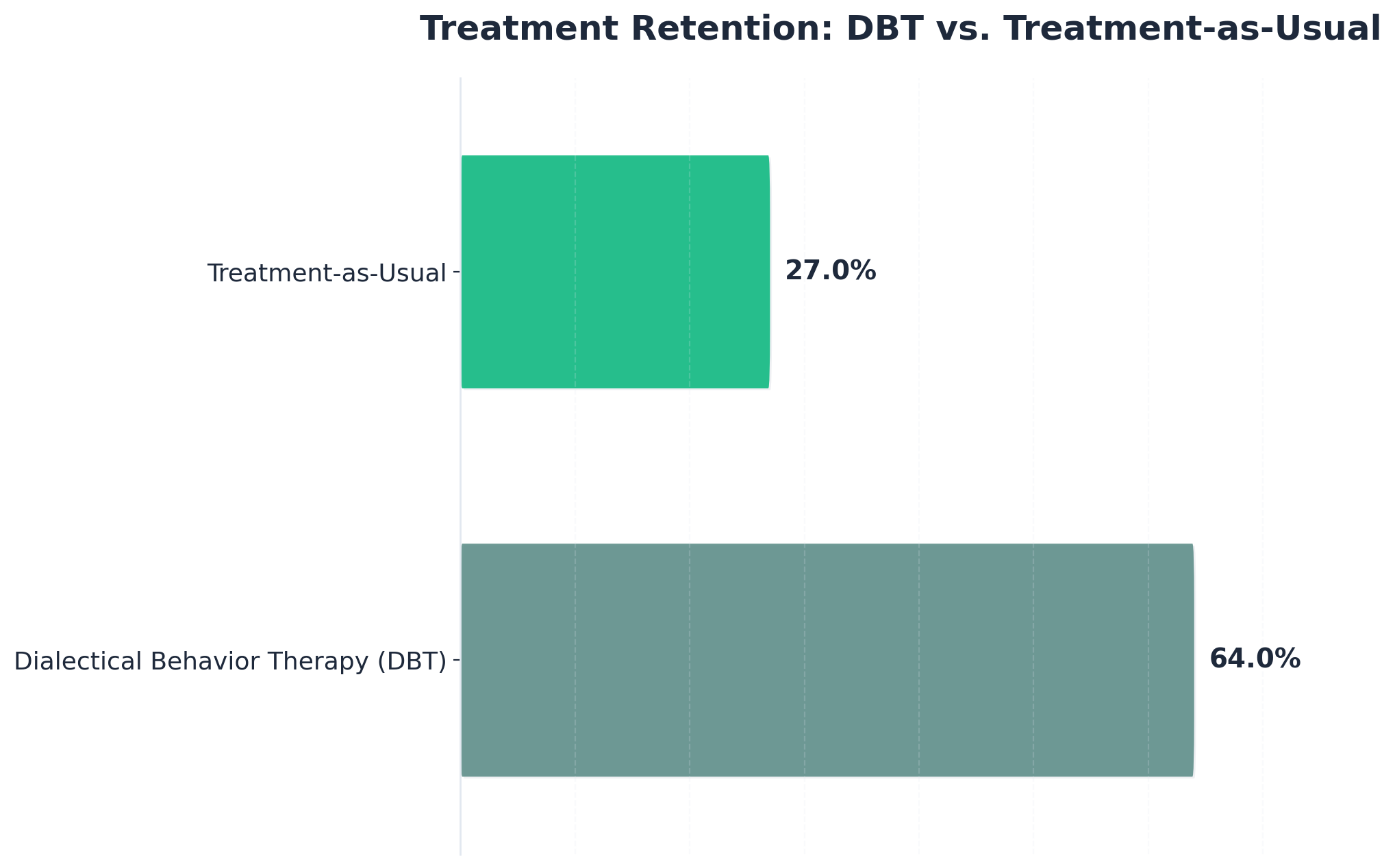
"Programs that include therapies like Dialectical Behavior Therapy (DBT) see much higher treatment retention; one study found 64% of people in DBT remained in treatment, compared to only 27% with standard care." 6
When people feel supported and have access to proven therapies, they’re more likely to stick with their recovery journey. Some seek outpatient care for business flexibility, while others focus on personal healing. Whichever path you choose, quality programs in the Portland area offer tailored services—from group therapy to medical monitoring—that adapt to your needs and daily life.
Practice This: Create your own "support bridge" diagram. List one way medical care, counseling, peer groups, and family can help keep you connected to recovery.
Skill Checkpoint: You’re ready for the next level when you can explain to someone why having access to multiple types of support makes an outpatient recovery program Portland area so effective.
IOP, PHP, and OP Programs Explained
What you’ll learn: In this section, you’ll get a clear breakdown of the three main types of outpatient care—Intensive Outpatient Programs (IOP), Partial Hospitalization Programs (PHP), and standard Outpatient Programs (OP). By the end, you’ll know how each level works and which path might fit your needs or schedule best.
Think of outpatient treatment like a ladder with different rungs. To help you decide which rung fits your current situation, review the comparison below:
Program TypeStructure & Time CommitmentBest Suited ForPHP (Partial Hospitalization)Highest structure. Meets most days/week for several hours daily.Those needing daily medical/therapeutic support but who can return home at night.IOP (Intensive Outpatient)Moderate structure. 3–5 days/week, often mornings or evenings.Balancing work, school, or family while receiving significant care.OP (Standard Outpatient)Flexible structure. Weekly or biweekly sessions.Stepping down from higher care or maintaining long-term stability.
Practice This: Match sample weekly calendars to each program type to see which fits your lifestyle best.
You’re ready for the next level when you can describe the differences between IOP, PHP, and OP to someone exploring an outpatient recovery program Portland area. Each service offers a personalized approach, letting people access the right mix of structure and independence for their recovery journey.
Evidence-Based Therapies in an Outpatient Recovery Program Portland Area
Recovery isn't built on hope alone—it's built on proven methods that have helped countless individuals reclaim their lives. Evidence-based therapies form the backbone of effective outpatient treatment, offering structured approaches that address the root causes of addiction and mental health challenges.
- Cognitive Behavioral Therapy (CBT): Stands as one of the most researched and effective interventions. It helps individuals identify negative thought patterns and develop healthier coping mechanisms. Through CBT, you learn to recognize triggers, challenge distorted thinking, and build skills that support long-term wellness.
- Dialectical Behavior Therapy (DBT): Offers powerful tools for emotional regulation, particularly for those struggling with intense feelings or relationship difficulties. This approach teaches mindfulness, distress tolerance, and interpersonal effectiveness—skills that translate directly into daily life.
- Motivational Interviewing (MI): Creates a collaborative space where ambivalence about change transforms into commitment. Rather than pushing someone toward recovery, this approach honors their autonomy while gently exploring the reasons change matters to them personally.
Group therapy adds another dimension, allowing individuals to share experiences, reduce isolation, and learn from peers who understand their journey. The combination of individual and group modalities creates a comprehensive support system that addresses recovery from multiple angles, meeting people exactly where they are in their healing process.
CBT and DBT: Building Lasting Coping Skills
What you’ll learn: In this section, you’ll see how Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) help people develop coping skills that last well beyond treatment. By the end, you’ll be able to identify practical tools these therapies offer and know why they are cornerstones of a strong outpatient recovery program Portland area.
CBT is like a mental toolkit for daily life. It helps people notice and change unhelpful thoughts, replacing them with realistic, positive habits. For example, someone might learn to challenge the belief, “I can’t handle stress without substances,” and build confidence in new ways to cope.
DBT goes a step further, blending skills for managing emotions, handling crisis moments, and improving relationships—especially helpful for those who feel overwhelmed or stuck in extremes. Research has shown that DBT can keep more people engaged in treatment: 64% of participants remained in care with DBT versus 27% with standard approaches. 6
Practice This: Write down a recent stressful situation. List one CBT skill (like thought-challenging) and one DBT skill (like deep breathing or using a support person) that could help you respond differently next time.
Skill Checkpoint: You’re ready for the next level when you can show how CBT and DBT skills apply to both business challenges (like work stress) and personal moments (like family conflict). Local providers include these therapies in their service offerings, supporting lasting success for every path.
Motivational Interviewing for Sustained Change
What you’ll learn: In this section, you’ll discover how Motivational Interviewing (MI) supports lasting change and why it’s a valued part of any high-quality outpatient recovery program Portland area. By the end, you’ll recognize how MI helps people move from feeling stuck to taking real, positive steps—whether for your own recovery or to help a loved one.
Motivational Interviewing is like having a guide who helps you find your own reasons to change, instead of being pushed or judged. Rather than telling someone what they "should" do, MI encourages open conversations that build confidence and highlight personal strengths. This gentle, respectful approach is especially powerful when people feel uncertain, helping them clarify their goals and stay motivated on tough days. Research shows that MI is proven to improve early treatment retention—a key factor in long-term recovery success. 7
Practice This: Write down one change you want to make in your life. Ask yourself: Why does this matter to me? What’s one small step I can take today? Notice how identifying your own reasons feels different from following someone else’s advice.
Skill Checkpoint: You’re ready for the next level when you can describe how MI could help with both business goals (like starting a new project) and personal goals (such as maintaining sobriety). Outpatient programs in the Portland area offer MI as part of their service offerings, giving clients the support and encouragement needed for genuine progress.
Recovery Starts With a Conversation
Whether you’re exploring recovery for yourself or seeking guidance for someone you care about, Coastal Recovery Partners is here to help. Our team offers trauma-informed, evidence-based support grounded in structure, compassion, and real connection—without pressure or judgment.
When you’re ready, we’ll meet you where you are and help you take the next step forward.
Integrated Care for Complex Needs
While these evidence-based therapies provide powerful tools, they work best when coordinated with comprehensive medical and social support. Recovery rarely follows a straight path, especially when individuals face multiple, interconnected challenges. Many people seeking treatment struggle with co-occurring mental health conditions, chronic medical issues, or social circumstances that complicate their journey.
Addressing these complex needs requires a coordinated approach where different specialists work together rather than in isolation. Integrated care—a model where multiple providers collaborate as a unified team rather than treating issues separately—brings medical professionals, mental health clinicians, case managers, and support specialists together with a focus on the whole person.
This collaborative approach ensures that treatment for substance use disorder doesn't happen in a vacuum, but considers physical health, psychological well-being, and practical life circumstances simultaneously. For example:
- Depression & Substance Use: Therapy addresses both conditions in tandem.
- PTSD & Addiction: Trauma-informed care recognizes how these conditions reinforce each other.
- Anxiety & Dependence: Coordinated psychiatric and addiction treatment prevents one condition from undermining progress in the other.
In practice, this means regular team meetings where providers review cases together, shared electronic health records that keep everyone informed of medication changes or crisis events, and coordinated treatment plans that all specialists contribute to and follow. This comprehensive approach prevents the fragmented care that often leads to gaps in treatment. When providers share information and coordinate their efforts, they can identify potential obstacles earlier, adjust treatment plans more effectively, and provide the wraparound support that complex cases demand.
Dual Diagnosis: Treating Co-Occurring Disorders
What you’ll learn: This section explains how dual diagnosis care treats both substance use and mental health conditions together. By the end, you’ll see why this integrated approach is vital—and how you can spot a program offering real support for complex needs.

Nearly half of those with addiction also live with depression, anxiety, or another mental health condition, making dual diagnosis far more common than many realize. 2
"Trying to address each concern separately is like patching a boat with two holes—unless both are fixed, you’ll keep taking on water."
Outpatient recovery programs in the Portland area bring mental health counselors and addiction specialists together as a team, so participants receive coordinated support in one place. This helps prevent relapse, improves emotional balance, and eases the daily challenges that can get in the way of progress.
Practice This: List two signs that a program offers true dual diagnosis care (for example, access to both therapy and medication management). Then, think about how this might help with work-life balance or personal goals.
Skill Checkpoint: You’re ready for the next level when you can explain to a friend why treating mental health and addiction at the same time leads to stronger, longer-lasting recovery outcomes. 2
Medication-Assisted Treatment Integration
What you’ll learn: This section shows how medication-assisted treatment (MAT)—now often called medications for opioid use disorder (MOUD)—fits into integrated care for addiction recovery. You’ll see how MAT works alongside therapy and support, and how to recognize programs that offer safe, evidence-based medication options. By the end, you’ll know why MAT can be a crucial part of a strong outpatient recovery program Portland area.
Think of MAT as an anchor that provides stability while you build new habits. Medications like methadone and buprenorphine help reduce cravings and withdrawal symptoms, making it easier to focus on therapy and daily responsibilities. Research has found that people with opioid use disorder who receive methadone or buprenorphine are 50% less likely to die from overdose compared to those not receiving these medications. 1
Quality outpatient programs in the Portland area integrate MAT with counseling, peer support, and medical monitoring, so clients get a full circle of care all in one place.
Practice This: Write down two ways medication could support your work or family life during recovery. Consider how having both medical and counseling support might help you reach your goals.
Skill Checkpoint: You’re ready for the next level when you can explain why MAT should be offered alongside therapy, and how this approach leads to safer, more stable recovery outcomes.
Trauma-Informed Care in an Outpatient Recovery Program Portland Area
Outpatient recovery environments should feel safe, welcoming, and free from triggers that could hinder healing. Trauma-informed principles recognize that many individuals struggling with substance use have experienced significant emotional or physical trauma, and creating supportive outpatient spaces plays a crucial role in their comfort and progress—even when clients aren't residing in the facility.
Effective trauma-informed outpatient spaces incorporate specific design and operational elements:
- Physical Environment: Natural lighting, calming colors, and comfortable furnishings that promote relaxation rather than institutional coldness.
- Privacy: Dedicated areas where individuals can process emotions without feeling exposed or vulnerable.
- Staff Training: Ensuring every interaction respects personal boundaries and acknowledges the courage it takes to seek help.
These environments also minimize power imbalances by involving clients in decisions about their care whenever possible. Flexibility in treatment schedules, choices in therapy modalities, and input on session planning help individuals regain a sense of control that trauma often strips away. Outpatient settings can offer flexible appointment times that accommodate work and family responsibilities, reducing the stress that rigid scheduling might create.
Outpatient facilities that embrace trauma-informed principles create spaces where healing can truly begin. Welcoming waiting areas with comfortable seating, private counseling rooms that ensure confidentiality, and accessible locations all contribute to reducing barriers to care. When the environment itself communicates safety and respect, individuals can focus their energy on recovery rather than self-protection. This foundation of trust and security becomes the bedrock upon which lasting change is built.
Why Trauma-Informed Care Matters
What you’ll learn: In this section, you’ll discover why trauma-informed care is essential in addiction recovery and how to spot programs that truly embrace this approach. By the end, you’ll recognize how a trauma-informed outpatient recovery program Portland area can support healing for both personal and business-focused clients.
When someone has experienced trauma, even small triggers can make it hard to trust others or feel safe in a treatment setting. Trauma-informed care addresses this by making sure every part of the program—from intake to therapy groups—is designed to avoid re-traumatization and honor each person’s story. Research shows that when programs use a trauma-informed model, people are more likely to stay engaged and have better outcomes in their recovery journey. 3
A simple analogy: imagine walking into a room where everyone cares about your comfort and listens without judgment—this is what a trauma-informed environment aims to provide. Outpatient recovery services in the Portland area put this into action by offering choices, building trust, and encouraging collaboration between clients and care teams.
Practice This: Think about one time you felt truly listened to. Write down what made that experience safe and positive. Compare it to how you’d want to be treated in a recovery program.
Skill Checkpoint: You’re ready for the next level when you can describe to someone else why trauma-informed care leads to higher engagement and better outcomes in outpatient settings.
Safety and Empowerment in Treatment
What you’ll learn: This section shows how true safety and empowerment are woven into daily life at a trauma-informed outpatient recovery program Portland area. By the end, you’ll be able to recognize how programs help clients regain a sense of control and confidence—key steps for lasting recovery.
Safety in treatment means more than just physical protection—it’s about emotional security, too. Trauma-informed programs make sure everyone feels welcome and respected, from the first phone call to each therapy session. For example, clients are offered choices in their care, like selecting group or individual sessions, setting personal goals, and having a say in their treatment plan. This sense of choice helps people feel empowered, not just like a patient, but an active partner in recovery. Research shows that when clients are treated with dignity and given real input, they’re more likely to stay engaged and see positive outcomes. 3
Practice This: Write down two ways you could ask for more choice or voice in a treatment setting—such as requesting a certain type of therapy or sharing your comfort needs with your counselor.
Skill Checkpoint: You’re ready for the next level when you can describe how safety and empowerment help both business-focused and personally motivated clients thrive in outpatient care.
Practical Steps to Begin Your Recovery Journey
Taking the first step toward recovery can feel overwhelming, but breaking the journey into manageable actions makes it more approachable. Start by acknowledging where you are right now—there's no shame in seeking support, and recognizing the need for change is already a significant achievement.
- Start with small, concrete actions. Reach out to a trusted friend or family member and share what you're experiencing. Research outpatient treatment options that align with your specific needs and lifestyle.
- Call local outpatient centers. Ask specific questions about their programs. Inquire about evening or weekend sessions if you're working or have family commitments—many outpatient facilities design schedules around typical work hours.
- Ask about virtual options. Virtual therapy can eliminate commute time and make consistent attendance easier. These outpatient approaches allow you to maintain your daily responsibilities while receiving the professional support you need.
- Create a simple daily routine. Include basic self-care practices like setting regular sleep times, preparing nutritious meals, or incorporating brief moments of mindfulness. These foundational habits support your overall well-being and create stability during challenging times.
- Connect with support groups. Meet others who understand what you're going through. Many outpatient programs incorporate group therapy, offering both professional guidance and peer support that provides validation and practical insights.
Remember that recovery isn't linear—setbacks are part of the process, not failures. The flexibility of outpatient care means you can adjust your treatment intensity as needed while maintaining the stability of your home environment. The path forward becomes clearer with each intentional step you take toward healing and growth.
Assessing Your Treatment Needs and Options
What you’ll learn: In this section, you’ll discover how to identify what you need from treatment and compare your options so you can make confident choices. By the end, you’ll know how to match your personal or professional priorities to the right outpatient recovery program Portland area.
Start by thinking about your daily responsibilities—work, school, family, or health. This helps you decide what kind of program fits your schedule. For example, Intensive Outpatient Programs (IOP) offer structured support without overnight stays, while standard outpatient care is even more flexible. Many programs in the Portland area also provide evening, weekend, and virtual sessions, meeting you where you are. Research highlights that flexible care models are helping more people access treatment while managing their commitments. 5
Practice This: Write down your top three needs (like session timing, support for mental health, or virtual options). Use this list when contacting providers to ask about their services and how they can tailor support for you.
Skill Checkpoint: You’re ready for the next level when you can clearly state your needs and confidently ask if a program’s services can meet them. Outpatient recovery programs in the Portland area are ready to help you find the right fit for your journey.
Navigating Insurance and Financial Barriers
What you’ll learn: This section explains how to navigate insurance and financial concerns when starting an outpatient recovery program Portland area. By the end, you’ll know practical steps to take, what questions to ask, and where to find support if coverage is a challenge.
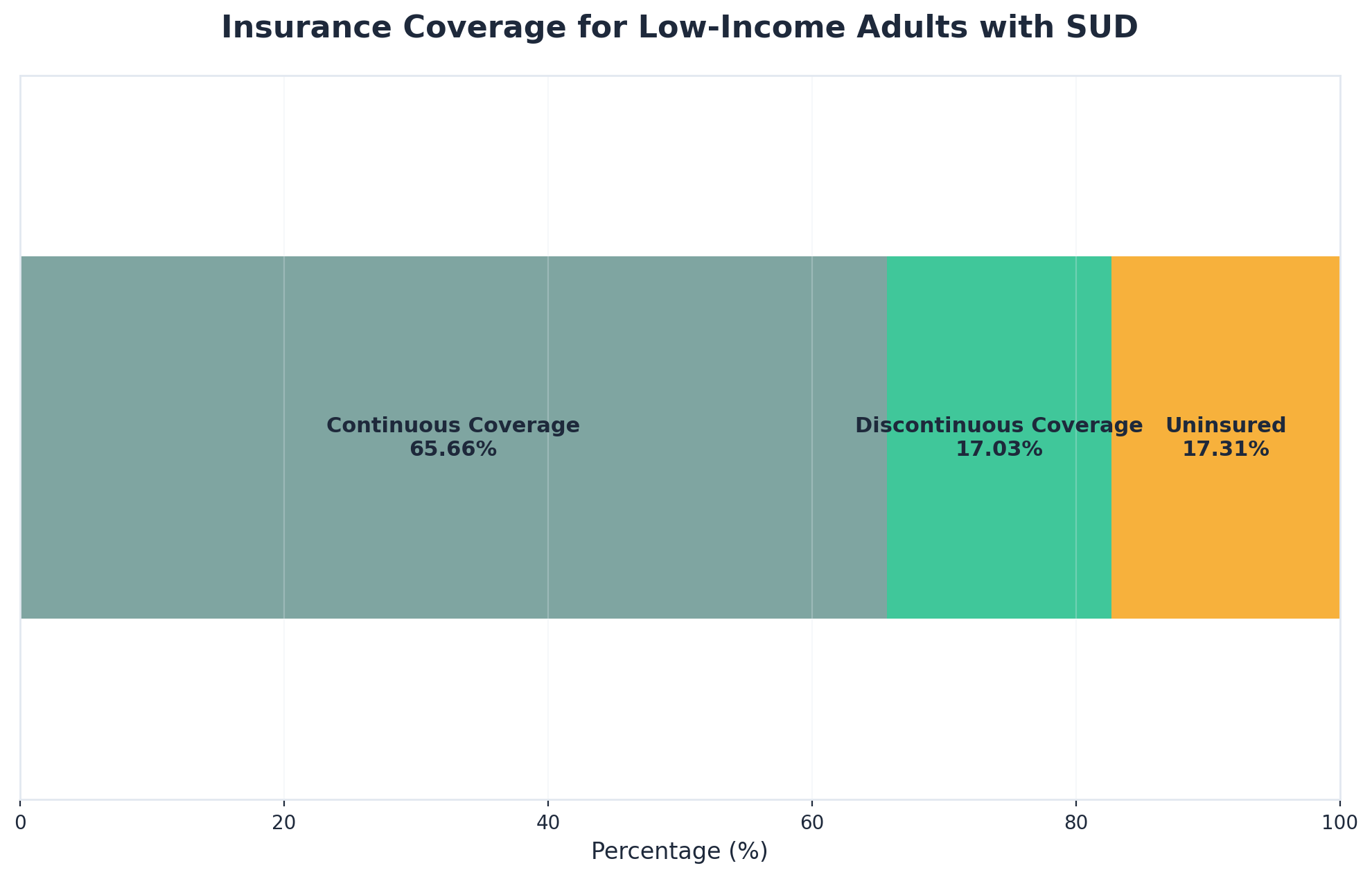
Understanding your insurance options is key to making treatment accessible. About one-third of low-income adults with substance use disorders either have gaps in coverage or no insurance at all—a barrier that often limits access to care. 5
The good news is that many outpatient programs in the Portland area offer help with verifying your benefits, exploring sliding scale fees, and connecting you to financial assistance resources. Service teams can walk you through your insurance plan, explain what’s covered, and help you plan for any out-of-pocket costs.
Practice This: Make a list of questions about insurance or payment (such as "Is my counselor in-network?" or "Are virtual sessions covered?"). Bring these to your first call or meeting with a provider.
Skill Checkpoint: You’re ready for the next level when you can clearly describe your insurance status and ask a program how they’ll support you in overcoming financial barriers to care.
Frequently Asked Questions
Can I work full-time while attending an outpatient program?
Yes, you can work full-time while attending an outpatient recovery program Portland area. Outpatient programs are specifically designed to fit around busy schedules, offering sessions in the early morning, evenings, or even on weekends to accommodate work and family obligations. Many programs also provide virtual therapy options, making it easier to participate without disrupting your job. Research shows that flexible care models like these are helping more people stay engaged in treatment while maintaining their daily responsibilities. 5
Service teams in the Portland area understand the importance of balancing career and recovery. They offer personalized scheduling and support, so you can focus on healing without sacrificing your professional goals. If you’re worried about balancing both, staff can help you create a plan that works for you and your employer.
How can family members support someone in outpatient treatment?
Family members play a vital role in supporting someone in an outpatient recovery program Portland area. Encouragement, open communication, and understanding make a real difference—simply checking in, listening without judgment, or attending family-focused sessions can boost motivation and help loved ones feel less alone. Many outpatient programs offer family education and counseling services, making it easier to learn about addiction, set healthy boundaries, and support positive changes at home. Research shows that when families are involved in treatment, substance use frequency drops by nearly 6% and recovery gains last longer. 4
Our team’s service offerings include family involvement as a core part of care, whether through structured family therapy, coaching, or regular updates. If you’re not sure how to help, ask the treatment provider about ways to participate or advocate for your loved one. Even small, consistent acts of support can strengthen recovery for everyone involved.
What happens if I relapse during outpatient treatment?
Relapse during outpatient treatment is not a sign of failure, but rather a common part of the recovery process. Outpatient recovery program Portland area teams understand that addiction is a chronic condition and setbacks can happen. If you experience a relapse, care providers will meet you with compassion, not judgment. The focus quickly shifts to helping you identify what led to the relapse and updating your treatment plan with added support—such as more frequent therapy, medication adjustments, or extra peer group sessions. Research supports this approach: shifting away from punitive responses to relapse and instead offering continued support leads to better long-term outcomes. 5
Service offerings in the Portland area are designed to help you get back on track, whether your goals are personal or professional. If you are struggling, reach out to your care team—they are ready to help you strengthen your recovery and find new strategies that work for you.
Is medication for addiction treatment something I'll need forever?
Medication for addiction treatment—such as methadone or buprenorphine—is not always something you’ll need forever. The length of time someone stays on medication depends on individual needs, progress, and goals. For some, medication is a short-term bridge; for others, it becomes a longer-term support to maintain stability and minimize cravings. Research shows that people who take these medications as prescribed are 50% less likely to die from overdose compared to those not receiving them. 1
Because addiction is a chronic condition, some people benefit from staying on medication for months or even years, while others may gradually reduce or stop with their provider’s guidance. The most important thing is to work closely with your care team in an outpatient recovery program Portland area. Their service offerings include regular check-ins and personalized plans, ensuring your treatment matches your unique journey and goals.
How do I transition from a higher level of care to outpatient treatment?
Transitioning from a higher level of care, such as residential or inpatient treatment, to an outpatient recovery program Portland area is a supportive and planned process. Most programs begin with a careful assessment to understand your needs, ensuring that your next steps are safe and well-matched to your progress. You’ll typically work with a care coordinator who helps you create a transition plan, which may include gradually stepping down treatment intensity, setting up regular outpatient sessions, and connecting you with ongoing support like therapy, medication management, or peer groups. Research emphasizes that coordinated transitions between levels of care improve treatment engagement and long-term recovery outcomes. 5
Service offerings at outpatient programs in the Portland area include dedicated staff to ease this transition, answer your questions, and help you stay connected to care. If you’re preparing for this step, don’t hesitate to ask about their process and how they’ll support you through the change—having a clear plan can make this move feel much more manageable and hopeful.
What if I don't have continuous health insurance coverage?
If you don’t have continuous health insurance coverage, you’re not alone—and it doesn’t mean you have to give up on getting help. In fact, about one-third of low-income adults with substance use disorders either have gaps in coverage or no insurance at all, which can make accessing treatment feel especially challenging. 5
The good news is that many outpatient recovery program Portland area providers understand these hurdles and offer practical solutions. Service teams can help you explore alternative payment options such as sliding scale fees, payment plans, and connections to local or state-funded assistance programs. They may also assist with insurance navigation if you regain coverage, or help you apply for Medicaid or other benefits. Don’t hesitate to ask about financial aid or community resources—support is available to help you start or continue your recovery, regardless of your insurance status.
Conclusion
Understanding the benefits of outpatient recovery programs empowers individuals to make informed decisions about their treatment journey during a critical life transition. While the variety of program options and therapeutic approaches might seem overwhelming at first, each element serves specific recovery needs and life circumstances. The key lies in recognizing that healing doesn't require putting life completely on hold—effective treatment can integrate seamlessly with daily responsibilities.
The flexibility to maintain work, family commitments, and personal routines while receiving evidence-based care creates a foundation for sustainable recovery. Programs that incorporate individual therapy, group support, medication management, and holistic approaches address the whole person, not just the addiction. Many individuals find that applying recovery skills in real-world settings as they learn them strengthens their ability to navigate challenges and build lasting resilience.
Whether someone needs intensive outpatient support or a less structured approach, the goal remains the same: achieving meaningful recovery while maintaining the life they've built. Outpatient treatment represents an investment in health, well-being, and a future free from addiction's grip. For those ready to explore their options and find a program that aligns with their unique situation, taking that first step toward outpatient care can open the door to transformation without requiring them to step away from everything that matters most.
References
- Medication-Assisted Treatment for Opioid Use Disorder. https://www.naco.org/resource/osc-mat
- Dual Diagnosis: Substance Abuse and Mental Health. https://www.helpguide.org/mental-health/addiction/substance-abuse-and-mental-health
- Feasibility and outcomes of a trauma-informed model of care in residential treatment for substance use. https://pubmed.ncbi.nlm.nih.gov/39566845/
- Family Involvement in Treatment and Recovery for Substance Use. https://pmc.ncbi.nlm.nih.gov/articles/PMC8380649/
- Healthcare coverage and service access for low-income adults with substance use disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC9086121/
- Dialectical Behavior Therapy for Substance Abusers. https://pmc.ncbi.nlm.nih.gov/articles/PMC2797106/
- Using Motivational Interviewing in Substance Use Disorder Treatment. https://library.samhsa.gov/sites/default/files/PEP20-02-02-014.pdf
- Gender and Use of Substance Abuse Treatment Services. https://pmc.ncbi.nlm.nih.gov/articles/PMC6470905/
- Treatment for Opioid Use Disorder: Population Estimates. https://www.cdc.gov/mmwr/volumes/73/wr/mm7325a1.htm
- Community Reinforcement and Family Training. https://www.ccsa.ca/sites/default/files/2019-04/CCSA-Community-Reinforcement-Family-Training-Summary-2017-en.pdf





